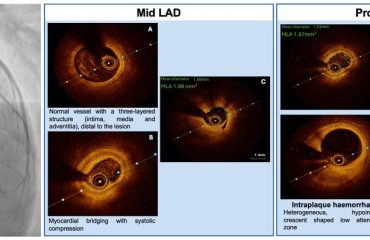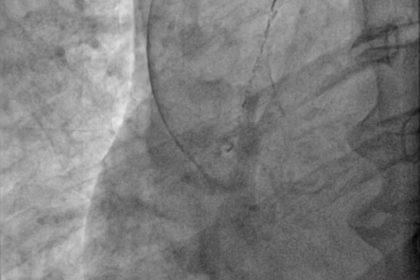
Descrição do caso: A 62-year-old female patient underwent elective percutaneous coronary intervention (PCI) following a non-ST-segment elevation myocardial infarction. Coronary angiography demonstrated a severely calcified aorto-ostial lesion of the right coronary artery (RCA), with a prominent calcium nodule in the coronary ostium. Lesion preparation was performed using a semi-compliant balloon, followed by a non-compliant balloon. However, delivery of a drug-eluting stent was unsuccessful due to severe calcification and inadequate lesion crossing. During manipulation, the stent became dislodged, remaining anchored distally within the RCA ostium and proximally extending into the ascending aorta. Initial retrieval attempts using a trapping-balloon technique and enhanced guide support were unsuccessful. The dislodged stent was ultimately retrieved using a dedicated snare system. Subsequently, PCI of the proximal RCA was performed after additional lesion preparation with intravascular lithotripsy, with successful implantation of a drug-eluting stent and an optimal final angiographic result. This case highlights the technical challenges posed by heavily calcified coronary lesions, the risk of stent dislodgement during complex PCI, and the importance of operator familiarity with bailout techniques, such as snare retrieval, for managing intravascular device complications.
Autores: Rita Louro, Gustavo Sá Mendes, Renato Fernandes, Lino Patrício
Centro de origem: Unidade Local de Saúde Alentejo Central